Published on June 15, 2018
Abstract
The purpose of this study is to look deeper into an electronic medical record (EMR) system to find inefficiencies within the overall charting process. Along with collecting observation data on nurses within the University of Missouri Hospital Intensive Care Unit, EMR activity log data was gathered from the EMR system through a real time measurement system (RTMS). By using the RTMS data, the total time of EMR usage for several designated charting activities was analyzed based on different levels of patient sickness and nurse experience. The results showed that there were several significant differences on the EMR documentation in this ICU. The comprehensive findings of this study will help point to areas where improvements can be made in order to optimize efficiency within the EMR charting process and increase time nurses spend in direct patient care, which should in turn increase patient safety as well.
Keywords: Intensive Care Unit, Electronic Medical Record, charting
Introduction
The University of Missouri Hospital Intensive Care Unit implemented electronic medical records in 1999 with the goal of increasing overall efficiency in the ICU. Although these electronic medical records have seemed to increase efficiency within the intensive care unit compared to the conventional paper method, there is still believed to be room for improvement (Kauffman, 2014). In this project, the first question that needs to be answered is why EMR charting has such a high percent time distribution and what factors may or may not affect it. Although past research has looked at the implementation of EMR systems and compared it to the paper charting system, this study looks deeper within the processes in the EMR system to discover how different factors affect the time spent in the EMR system. By doing so, the charting activities that are causing the inefficiency can be optimized in order to maximize the overall efficiency within the entire EMR charting process and increase time nurses spend in direct patient care.
Data Collection
For five months, two members of our research team collected twenty-eight days (7 am to 7 pm) of observation data and EMR log data from ICU nurses at the University of Missouri Hospital Intensive Care Unit. A Real-Time Measurement System (RTMS) marked the time duration for every completed EMR activity during their shifts. RTMS also provided all of the log data from the nurses’ EMR charting. The RTMS data was then used to create sequence diagrams that contained the location, duration, and time of each EMR activity that the ICU nurses performed. The time duration for all of the EMR activities was used as a basis for the preliminary data analysis. In addition, our team collected the Sequential Organ Failure Assessment (SOFA) scores, Charlson Comorbidity Index (CI) scores, and each nurse’s working experience in ICU during the data collection. The Charlson Comorbidity Index predicts the ten-year mortality rate for a patient who may have comorbid conditions (Charlosn et al., 1987). The Sequential Organ Failure Assessment is a measure “to objectively quantify the degree of dysfunction/failure of each organ daily in critically ill patients” (Ceriani et al., 2003). Years of nurse work experience, CI score, and SOFA score were all used as factors for defining different levels of patient sickness and nurse experience.
Hierarchical Task Analysis
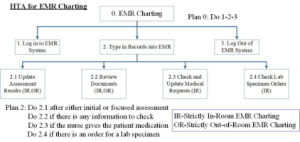
Although there are many studies related to the effects of EMR implementation and its efficiency in hospitals, few studies have looked into the detailed workflow in the EMR systems to determine the inefficient processes and how to improve them. To understand the ICU nurse’s EMR documentation workflow, the EMR data was split into several categories by using the hierarchical task analysis (HTA) method. As Annett (2003) states, “The process of HTA is to decompose tasks into subtasks to any desired level of detail…. The overall aim of the analysis is to identify actual or possible sources of performance failure and to propose suitable remedies, which may include modifying the task design and/or providing appropriate training.” HTA was used to diagram of all of the tasks and subtasks completed during EMR charting processes. Figure 1 shows one of the plans related to the four main areas of EMR charting input based on RTMS data: (1) update assessment results, (2) review documents, (3) check and updating medical requests, and (4) check lab specimen orders.
Procedure for Analysis
By using the HTA and RTMS data, the ICU nurses’ EMR activities were classified into five main EMR categories: in-room assessment, out-of-room assessment, medication, lab specimen, and others. The in-room assessment category includes every activity charted inside the patient room that is related to patient assessment, and the out-of-room assessment category is the same with the lone exception of the charting being conducted outside of the patient room. The medication category is comprised of all charting activities related to scanning and administering medication to patients. Similarly, the lab specimen category contains every charting activity related to scanning and transporting bloodwork and other lab specimens. This includes a nurse scanning the barcode on the patient’s tag, scanning the specimen container’s barcode, and then scanning the container’s barcode again once the lab specimen has been collected. Lastly, ‘others’ category includes every EMR charting activity that is not related to the other four RTMS categories, which mainly consists of nurses reviewing documents or previous orders within the EMR system.
During the data analysis, the times for each occurrence of EMR usage were marked and distributed into the five categories. After that, an average process time of each category was calculated. In this study, SOFA, CI, and nurse experience were used as independent variables to understand the effects of the levels of patient sickness and nurse experience on these five main EMR activities. Nurse experience is based on how many years nurses have worked in an intensive care unit. The levels of patient sickness are given by the SOFA and CI scores that each represent different levels of risk of death for each patient. Those scores were then separated into “high” and “low” categories based on the mean value for both metrics. A Charlson Comorbidity Index score of less than or equal to four was categorized as “low,” and a SOFA score of less than or equal to seven was categorized as “low.” For the nurse experience, if a nurse had more than two years of work experience in the ICU, then we considered that she or he was an experienced nurse. After categorizing the factors and data for the RTMS analysis, a one-way ANOVA test was conducted to show how both patient sickness and nurse experience contribute to the total time spent on EMR documentation.
Results
After creating the ANOVA tables for the total time, several significant differences for each factor were found. Determining whether there is a significant difference or not is a result of rejecting the null hypothesis when the alpha value is 0.05. In order to reject the null hypothesis, the p-value for the factor must be less than or equal to 0.05. In constructing the ANOVA tables, the first step was to test for any significant differences between the levels of the factors for the total charting time in the EMR system. Table 1 shows the ANOVA results for the in-room assessment total time, where the CI score has p=0.057 and the nurse experience has p<0.001. The difference in the CI score levels is close to being significant, so it is included with the other significant scores for this part of the analysis. The mean time for nurses whose patients had low CI scores is greater than those who had high CI scores, and the mean time for nurses with high experience is greater than those with low experience.
Table 1. ANOVA Results for Total Time for In-Room Assessment Charting
| Factor | Level | N | Mean | StDev | F | P |
| CI | Low | 19 | 36.00 | 18.64 | 3.97 | 0.057 |
| High | 9 | 21.39 | 16.90 | |||
| SOFA | Low | 17 | 27.94 | 17.59 | 1.36 | 0.254 |
| High | 11 | 36.50 | 20.98 | |||
| Nurse Experience | Low | 19 | 23.21 | 16.80 | 16.85 | <0.001 |
| High | 9 | 48.39 | 10.56 |
Table 2 shows the ANOVA results for the out-of-room assessment total EMR documentation time, in which the difference in the total times between the nurse experience levels is significant with a p=0.047. Contrary to the in-room assessment total time, nurses with low experience use the EMR system for much longer when charting for an assessment outside the patient room. Table 4 shows the ANOVA results for the total time spent charting about collecting lab specimens, in which the difference in the total times between the CI scores is significant with p=0.047. Nurses with patients who had low CI scores charted significantly more for collecting lab specimen than those with high CI scores. Table 5 shows the ANOVA results for charting for the designated ‘others’ category, in which the difference in the total times between the nurse experience levels is significant with p=0.014. Nurses with high experience charted more miscellaneous data in the EMR system than nurses with low experience.
Table 2. ANOVA Results for Total Time for Out-of-Room Assessment Charting
| Factor | Level | N | Mean | StDev | F | P |
| CI | Low | 19 | 42.47 | 23.95 | 1.29 | 0.266 |
| High | 9 | 54.00 | 27.45 | |||
| SOFA | Low | 17 | 44.71 | 16.02 | 0.14 | 0.708 |
| High | 11 | 48.5 | 36.0 | |||
| Nurse Experience | Low | 19 | 52.63 | 15.36 | 4.35 | 0.047 |
| High | 9 | 32.6 | 36.1 |
Table 3. ANOVA Results for Total Time for Medication Charting
| Factor | Level | N | Mean | StDev | F | P |
| CI | Low | 19 | 14.21 | 5.05 | 2.15 | 0.155 |
| High | 9 | 11.22 | 5.02 | |||
| SOFA | Low | 17 | 12.03 | 5.37 | 2.58 | 0.120 |
| High | 11 | 15.14 | 4.34 | |||
| Nurse Experience | Low | 19 | 12.79 | 5.79 | 0.46 | 0.502 |
| High | 9 | 14.22 | 3.50 |
Table 4. ANOVA Results for Total Time for Lab Specimen Charting
| Factor | Level | N | Mean | StDev | F | P |
| CI | Low | 19 | 3.697 | 3.763 | 4.36 | 0.047 |
| High | 9 | 1.000 | 1.118 | |||
| SOFA | Low | 17 | 2.662 | 4.055 | 0.10 | 0.750 |
| High | 11 | 3.091 | 2.119 | |||
| Nurse Experience | Low | 19 | 2.750 | 3.836 | 0.03 | 0.859 |
| High | 9 | 3.000 | 2.345 |
Table 5. ANOVA Results for Total Time for Other Charting
| Factor | Level | N | Mean | StDev | F | P |
| CI | Low | 19 | 29.50 | 14.17 | 0.02 | 0.885 |
| High | 9 | 28.56 | 19.37 | |||
| SOFA | Low | 17 | 26.21 | 15.34 | 1.61 | 0.215 |
| High | 11 | 33.82 | 15.71 | |||
| Nurse Experience | Low | 19 | 24.34 | 14.44 | 6.93 | 0.014 |
| High | 9 | 39.44 | 13.58 |
Discussion and Conclusion
In summary, this study showed that the RTMS data could be used as an important tool to improve the EMR charting process in the ICU. Several takeaways can be made from the results of the RTMS analysis. First, nurses with higher experience spend more time in the EMR system for in-room assessment charting, but spend less time in the EMR system for out-of-room assessment charting. This means that nurses with high experience prefer to chart patient assessments inside the patient room, likely because they are trying to chart immediately after an assessment is performed instead of waiting until a later time. Additionally, nurses with nurses with low experience prefer to wait to chart assessments until they are outside the patient room. Second, nurses with high experience charted inputs within the “other” category for a much longer time than nurses with low experience. A survey of responses on the amount of computer training for each nurse conducted by Robert Eley et al. (2008) concluded that 70.6% of nurses who have worked as a nurse for five years or less have had formal computer training, whereas only 23.7% of nurses who have worked as a nurse for five years or longer have had formal computer training. This can cause non-value added tasks to appear in the RTMS data, which would explain the large total time that highly experienced nurses spend charting for the designated “other” category. Third, for charting about collecting lab specimens, nurses with patients who have low CI scores chart much longer than those with high CI scores. In a study conducted by Alexander Rusanov et al. (2014), they looked at the American Society for Anesthesiologists Physical Status Classification (ASA class) for patients to determine if the health of patients affected the number of days where laboratory results were taken and medications were ordered. In this study, they found that ASA Class 4 patients, who were designated as the most sick, had 5.05 times the number of days with laboratory results as ASA Class 1 patients, who were designated as the least sick. This contradicts the corresponding result from the RTMS analysis relating CI scores to charting about lab specimens, so further tests should be done to verify these results and find the cause for that significant difference.
Although significant results were found that help to fill previous research gaps, there will always be more that can be done in terms of improving the electronic medical record system in the ICU. One test that would prove to be useful would be to determine the average time for each task within the EMR system to see which tasks are taking up the most amount of the nurse’s time. The averages then could then be tested with nurse experience and patient sickness to see if such factors are affecting EMR usage. From there, the EMR programming or ICU procedures could be improved to help cut down EMR usage time. Another component of the research that could be developed is a simulation model of the ICU. A simulation of the ICU would directly show how different tasks in the EMR system affect the nurse’s EMR usage over a long period of time. It would also show the value that would be gained from improving the tasks that are causing inefficiencies within the EMR system. Another aspect of the experiment that could expand is the control variable of where to test for EMR usage time. Instead of just looking at the ICU, the entire hospital or even multiple hospitals could be tested for EMR usage time. Although much more equipment and time would have to be invested, it would supply a much larger set of data to test, which would give better insight into inefficiencies within the EMR system in different environments. This would also help to improve EMR usage times not only in the University of Missouri Hospital but hospitals everywhere.
Another way that the research could be expanded is by looking at the limitations that were faced within this research project. One limitation was the data set that was used for this experiment since the data was collected from a previous experiment. To improve the data set, an independent study could be done with a larger sample size that focuses primarily on the tasks within the EMR system. This would allow the results to be drawn from a better data set that has different factors as independent variables. Another minor limitation was the RTMS data that was collected. Although the RTMS data was collected for every task that was charted within the EMR system, the data was difficult to interpret at times and there were several gaps in the log data that could not be explained. These gaps heavily affected the sample size for our experiment, so better consistency within the RTMS system would allow for a larger and more accurate data sample.
Benjamin Smith is a Senior at the University of Missouri majoring in Industrial Engineering.